Filip Van hulle, General Manager and pharmacist at Kaneka Pharma Europe, explains: this creates the energy our body needs to function and survive. Nick Lane’s “Power, Sex, Suicide: Mitochondria and the Meaning of Life,” states that long life relies on the relation between cellular energy, free radicals and their formation within mitochondria.1
“In terms of consumer awareness, the link between mitochondria and health is entering an important educational growth phase,” states SPINS (sales data).2 In an expanding and ageing world population, the demand for products that enable consumers to remain active and vital for longer is definitely here to stay.
Energy for life
During oxidative phosphorylation, the final stage of cellular respiration, mitochondria need oxygen to break down pyruvate and synthesise ATP (Figure 1). Water and carbon dioxide are generated as end products. In the cristae within mitochondria, real cellular energy is made via the complexes of the electron transport chain (ETC).
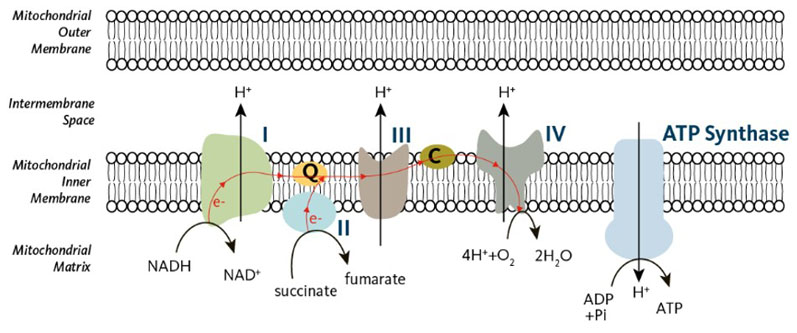
Figure 1: The ETC is organised into five transmembrane protein complexes (I–V); there are approx. 1000 ETC/mitochondria3
To explain the phenomenal work rate of mitochondria, a healthy person at rest produces their body weight in ATP every day. During maximal exercise, this number can increase to 0.5–1.0 kg per minute. The average cell uses 10 billion ATP molecules per day and, as such, a typical adult needs 3.0 × 1025 ATP molecules.4
Each ATP moiety needs to be recycled from ADP approximately 1000 times per day. There is about 250 g of ATP in a human body; this represents about 4.25 watts, the equivalent of the energy in an AA battery. Every day, therefore, a healthy person produces a remarkable 1200 watts.5
Mitochondria produce about 90% of the biochemical energy that cells need to survive.6 Because the body cannot store ATP, the mitochondria must function all the time. When mitochondria and the ETC do not function normally, serious diseases tend to manifest themselves.
These range from genetic disorders that affect how mitochondria are made to acute injuries such as heart attack and stroke, as well as chronic complaints such as obesity, diabetes and degenerative conditions such as Parkinson’s and Alzheimer’s diseases.
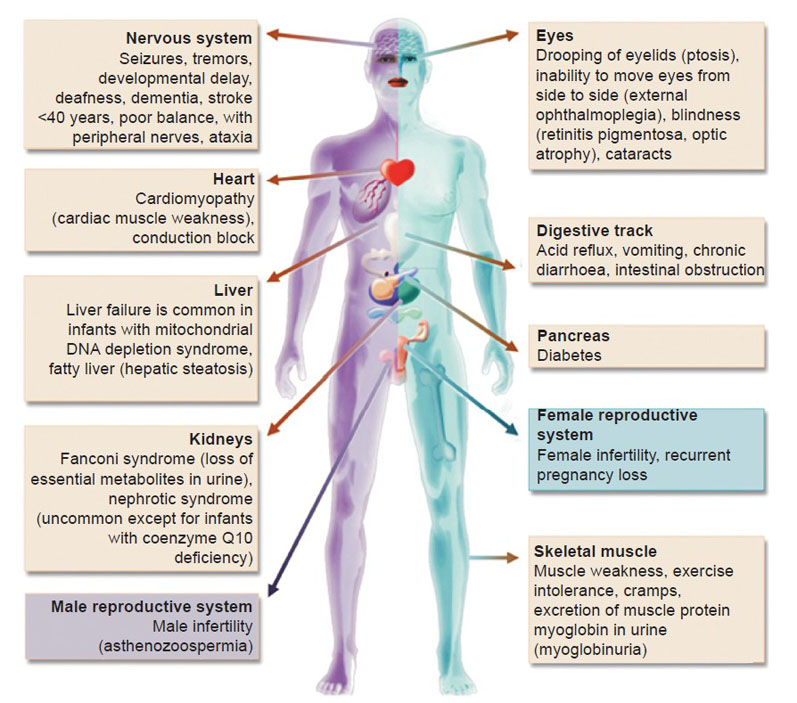
Figure 2: Mitochondria are connected to many pathologies7
Negative impact and health risks
It has been documented that the number of mitochondria decreases with age and disease. Age-associated decline in mitochondrial function — such as a 40% reduction in oxidative and/or phosphorylation activity in the elderly — contributes to insulin resistance and a loss of skeletal muscle.
Mitochondria in type 2 diabetics and obese subjects were found to be smaller when compared with those of healthy people.8,9 Even if this field is not fully explored yet, drugs also have an impact on mitochondria. For example, Medsafe, the New Zealand Medicines and Medical Devices Safety Authority, offers official guidelines titled: “Mitochondrial Disorders: Medicines to Avoid.”10
Recreational drugs such as cocaine, methamphetamines and alcohol are also problematic, as are various environmental chemicals.11 Other mitochondrial poisons include, for example, heavy metals (mercury, cadmium, etc.), aluminium, sulphites (red wine) and many more.
Lipophilic compounds such as polycyclic aromatic hydrocarbons (PAHs) have been found to accumulate in the lipid content of mitochondrial membranes.12 Carbon monoxide and cyanide act as Complex IV inhibitors and can cause rapid death.13
Counteracting with a healthy diet
Besides the negative effects of age, disease and chemical agents, there are other substances that, by contrast, can support the health and activity of mitochondria.14 In particular, vitamins and micronutrients should be included in any balanced daily diet (Figure 3).
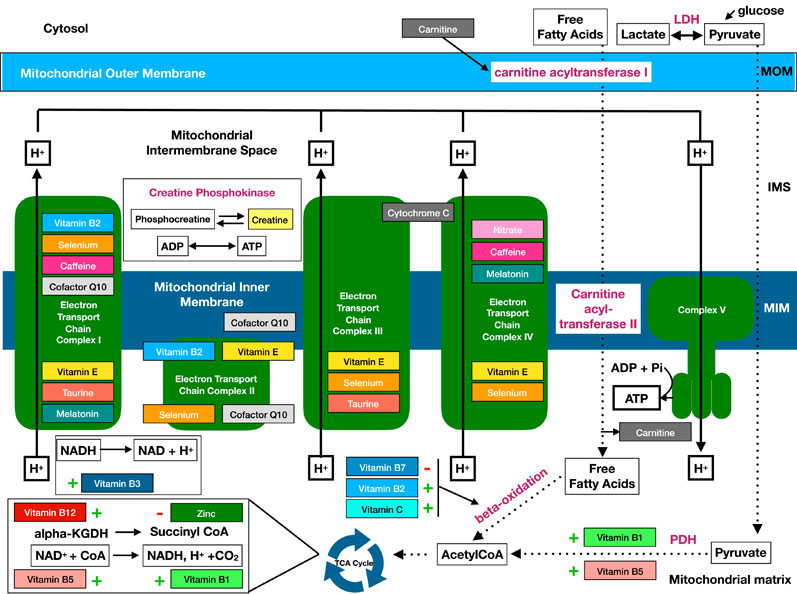
Figure 3: Feeding mitochondria: nutritional components may improve critical illness convalescence15
Niacin (vitamin B3) is an essential part of NADH and NADP synthesis and both pantothenic acid (vitamin B5, part of coenzyme A) and pyridoxal phosphate (vitamin B6) are crucial for many metabolic reactions. The latter is one of the most important vitamins in terms of mitochondrial function; likewise, cobalamin (vitamin B12) deficiency has been associated with decreased mitochondrial respiration and energy production.
Also, 30–50% of cellular folates are located in the mitochondria. As well as vitamins, certain herbs have also been shown to positively affect mitochondria.
Another study focused on nutrients or combinations that lead to increased ATP. It was found that the combination of coenzyme Q10 (CoQ10), vitamin C, vitamin E, vitamin B2/B1/B3, vitamin K and carnitine improved ATP synthesis in the lymphocytes of patients with QXPHOS disorders.
When nutrients were individually tested, there was no significant increase in ATP synthesis except when they were combined with CoQ10. Furthermore, the increase in ATP synthesis derived from a combined treatment was not significantly different to that obtained from a single treatment of CoQ10 alone. The researchers could therefore demonstrate that CoQ10 is the critical component in ATP synthesis.16
Ubiquinol as a key nutrient for mitochondria
The ETC is the most important part of the cellular energy or ATP creation pathway. Other vitamins and minerals may be involved in energy generation, helping to produce molecules for the ETC, but CoQ10 is the only element that is essential and is responsible for the transport of electrons (Figure 4).
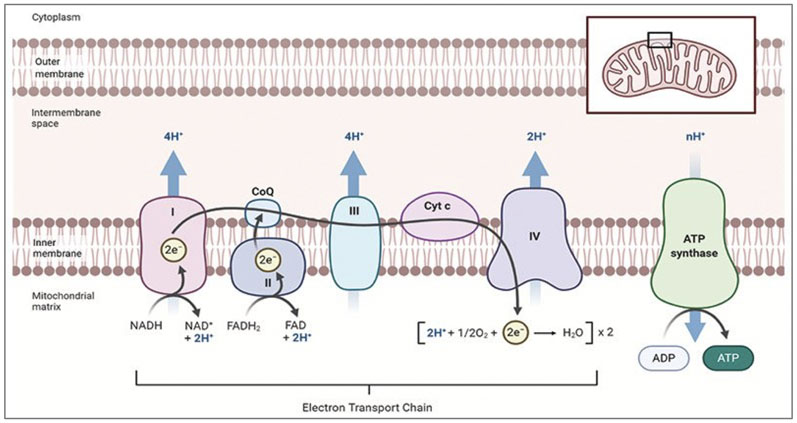
Figure 4: CoQ10 in the electron-transport-chain
Cellular energy production occurs in four stages and CoQ10 is involved in all of them. Complex I is essential; if it doesn’t function properly, no energy can be generated.17 Furthermore, this complex is most affected by ageing and is the primary site where free radicals are produced.18
Ubiquinol enables the process to skip Complex I and II and proceed directly to Complex III to produce ATP. A proton gradient is required for effective ETC activity and, with ubiquinol, more protons are pumped. Therefore, ubiquinol enhances cellular energy generation and reduces free radical production.19
Moreover, it “detoxifies” superoxide anion radicals, as well as peroxyl radicals, and regenerates alpha-tocopherol.20,21 Nitric oxide (NO) is produced by nearly every type of cell in the human body and inside mitochondria.
It can be converted to peroxynitrite and further ATP reduction; but, mitochondrial ubiquinol protects against peroxynitrite-mediated damage and restores mitochondrial function and integrity.22 As a substance with a low molecular weight (865 g/mol), ubiquinol can pass through mitochondrial membranes (unlike CoQ10).23
Supplementation with ubiquinol
It is understood that most diseases target certain organs; however, there is a growing belief that the origins of many ailments exist within the mitochondria. Ubiquinol is a fundamental agent of mitochondrial respiration, ATP production and optimal working metabolism.
This is amply demonstrated by the fact that both processes decrease by approximately 10% every 10 years (Figure 5). But, as proven, the age-related reduction in mitochondrial respiration and ATP production can be counteracted by ubiquinol.24
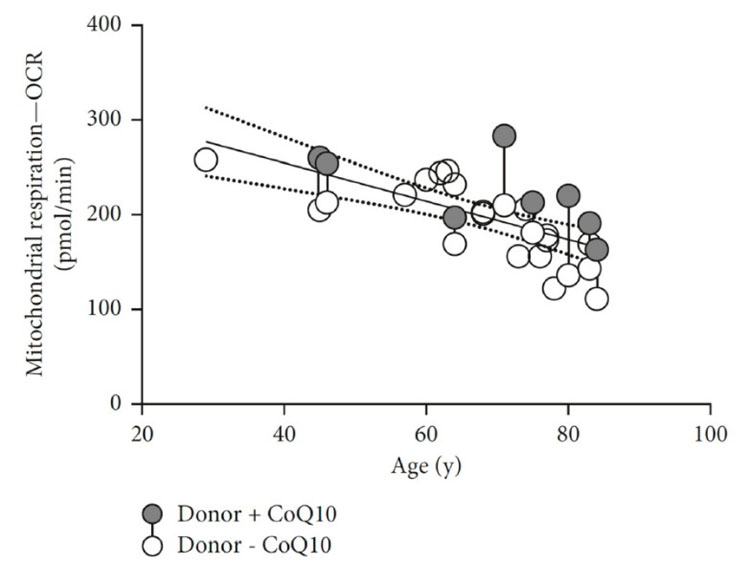
Moreover, a randomised double-blind, placebo-controlled clinical trial involving supplementation with 200 mg ubiquinol/day for 1 month showed an increase in both the number and health condition of mitochondria thanks to increased gene expression.25
Figure 5: The grey circles show ubiquinol treated samples, the white circles are untreated samples and the connected circles represent samples from the same donor
The recommended daily intake of ubiquinol is typically 100 mg a day; this may vary, however, according to individual needs, such as balancing out a disease-induced deficiency, the use of certain drugs, increased oxidative stress or intense sport. As ubiquinol is fat-soluble, taking it with food is advised. Some researchers recommend a dosage as high as needed to reach plasma levels of 3 µg/mL.
Support for the organism and healthy ageing
With proper supplementation, elderly people can replenish their cellular energy levels. Given that mitochondria are crucial for healthy ageing and ubiquinol is the key nutrient that can “unlock the vitality door,” supplementing an ageing society is more important now than ever before. And, with the increasing awareness of the versatility and benefits of micronutrients, a broader range of application options for nutritional products is on the horizon.26
References
- N. Lane, Power, Sex, Suicide: Mitochondria and the Meaning of Life (Oxford University Press, Oxford, UK, 2005).
- https://www.spins.com/tag/mitochondria/.
- https://lpi.oregonstate.edu/mic/dietary-factors/coenzyme-Q10.
- http://openwetware.org/wiki/BioNumber_Of_The_Month.
- S. Törnroth-Horsefield and R. Neutze, “Opening and Closing the Metabolite Gate,” Proc. Natl Acad. Sci. USA 105(50), 19565–19566 (2008).
- K Carvajal and R. Moreno-Sánchez, “Heart Metabolic Disturbances in Cardiovascular Diseases,” Arch. Med. Res. 34(2), 89–99 (2003).
- N.A. Khan, et al., “Mitochondrial Disorders: Challenges in Diagnosis and Treatment,” Indian J. Med. Res. 141, 13–26 (2015).
- K.F. Petersen, et al., “Mitochondrial Dysfunction in the Elderly: Possible Role in Insulin Resistance,” Science 300, 1140–1142 (2003).
- D.E. Kelley, et al., “Dysfunction of Mitochondria in Human Skeletal Muscle in Type 2 Diabetes,” Diabetes 51, 2944–2950 (2002).
- https://medsafe.govt.nz/profs/PUArticles/June2017/MitochondrialDisordersMedicinestoAvoid.htm.
- S. Manzo-Avalos and A. Saavedra-Molina, “Cellular and Mitochondrial Effects of Alcohol Consumption,” Int. J. Environ. Res. Public Health 7(12), 4281–4304 (2010).
- J.M. Backer and I.B. Weinstein, “Interaction of Benzo(a)pyrene and its Dihydrodiol-Epoxide Derivative with Nuclear and Mitochondrial DNA in C3H10T 1/2 Cell Cultures,” Cancer Res. 42, 2764–2769 (1982).
- J. Ninomiya-Tsuji, et al., “Mitochondrial Dysfunction” in R.C. Smart and R. Hodgson (Eds.), Molecular and Biochemical Toxicology, Fourth Edition (John Wiley & Sons, Inc., London, UK, 2008).
- B.N. Ames, et al., “Mineral and Vitamin Deficiencies Can Accelerate the Mitochondrial Decay of Aging,” Mol. Aspects Med. 26(45), 363–378 (2005).
- E. Wesselink, et al., “Feeding Mitochondria: Potential Role of Nutritional Components to Improve Critical Illness Convalescence,” Clinical Nutrition 38(3), 982–995 (2019).
- B.J. Marriage, et al., “Cofactor Treatment Improves ATP Synthetic Capacity in Patients with Oxidative Phosphorylation Disorders,” Mol. Genet. Metab. 81(4), 263–272 (2004).
- A.V. Kuznetsov, et al., “Application of Inhibitor Titrations for the Detection of Oxidative Phosphorylation Defects in Saponin-Skinned Muscle Fibers of Patients with Mitochondrial Diseases,” Biochim. Biophys. Acta 1360(1997), 142–150 (1997).
- G. Lenaz, et al., “Mitochondrial Complex I Defects in Aging,” Mol. Cell. Biochem. 174(1997), 329–333 (1997).
- R. Cervellati and E. Greco, “In Vitro Antioxidant Activity of Ubiquinone and Ubiquinol Compared to Vitamin E,” Helv. Chim. Acta 99(1), 41–45 (2016).
- L. Ernster and P. Forsmark-Andrée, “Ubiquinol: An Endogenous Antioxidant in Aerobic Organisms,” Clin. Investig. 71(8 Suppl.), S60–S65 (1993).
- V. Kagan, et al., “Antioxidant Effects of Ubiquinones in Microsomes and Mitochondria are Mediated by Tocopherol Recycling,” Biochem. Biophys. Res. Commun. 169(3), 851–857 (1990).
- F. Schöpfer, et al., “Oxidation of Ubiquinol by Peroxynitrite: Implications for Protection of Mitochondria Against Nitrosative Damage,” Biochem. J. 349, 35–42 (2000).
- L. García-Corzo, et al., “Ubiquinol-10 Ameliorates Mitochondrial Encephalopathy Associated with CoQ Deficiency,” Biochim. Biophys. Acta 1842, 893–901 (2014).
- D. Schniertshauer, et al., “Age-Dependent Loss of Mitochondrial Function in Epithelial Tissue Can be Reversed by Coenzyme Q10,” J. Aging Res. (2018): 6354680.
- C. Pérez-Sánchez, et al., “Ubiquinol Effects on Antiphospholipid Syndrome Prothrombotic Profile: A Randomized, Placebo-Controlled Trial,” Arterioscler. Thromb. Vasc. Biol. 37(10), 1923–1932 (2017).
- J.D. Hernández-Camacho, et al., “Coenzyme Q10 Supplementation in Aging and Disease,” Front. Physiol. 9, 44 (2018).
